AirCARE 1 case study: Covid-19 patient transfer

Denise Waye of AirCARE1 reports on a Covid patient mission in which the patient arrived in a very different condition to what had been expected, forcing the air medical crew to take swift and decisive action
AirCARE1 was called by family members to transport a 67-year-old male from a remote city in central Mexico to the state of Delaware in the US. This gentleman was a wealthy businessman who operated successful businesses in both Mexico and the US. He had recently travelled to Mexico to attend to his business, where he contracted Covid-19.
The family stated this patient had been in the hospital in Mexico for three weeks, and the facility did not have the means to properly manage his care. The family needed to get him to the US for better treatment as soon as possible.
Communication problems
Prior to transport, our nurse attempted multiple times to contact the attending physician in Mexico to receive a patient report, only to be told by the physician that the patient was very ill, and not fit to fly. The physician did state the patient was indeed Covid positive, and was on a ventilator. No further information could be obtained.
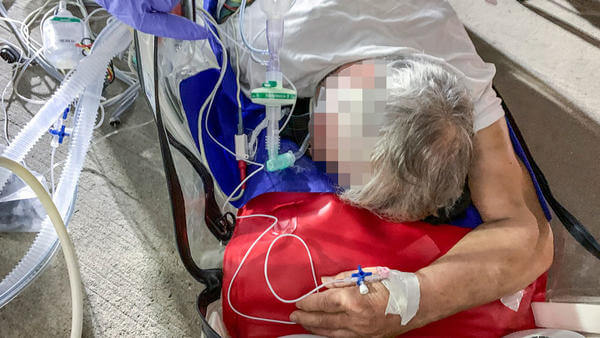
The family was desperate to move the patient so he could receive better care. We decided to utilize a family member as a resource to help determine the severity of the patient’s condition. The AirCARE1 nurse was able to contact the son, who was at the hospital with his father. By utilizing the son as a resource, we were able to obtain the information we needed, as well as the patient’s vital signs and ventilator settings via pictures he sent to us.
Based on further discussions with the family, our medical team, medical director, and these pictures, we determined that while the patient was critical, our team was fully capable of performing this transport.

Risk assessment
Before the flight, our team performed an operational risk management (ORM). This tool provides the medical crew the means to evaluate the acuity and any associated risks for the patient by assigning a risk value. Our ORM indicated a high, but acceptable, risk for this flight through risk mitigation measures.
We mitigated this risk by adding an additional medical crewmember to the team and utilizing dual HEPA filters on our ventilator to prevent any contamination to our team, as the patient was too large to fit inside our isolation chamber.
Other risk factors included that the patient was coming from a remote location in central Mexico, we had limited information on the patient’s condition, and there were probably other unknown factors we might not be aware of. We also were not sure of the extent of interventions the patient initially may require, and wanted to err on the side of caution.
Furthermore, since the patient was quite a distance away from the airport and had to be transported through mountainous terrain, it was not feasible for our medical crew to go to his bedside. While this is never the most desirable option, we mitigated this risk by contracting with a ground ambulance operator that stated they would have a physician onboard who would be able to manage the ventilated patient.
By taking all of these risk factors into account, we felt we had mitigated the risk of this flight to an acceptable level.

Mission ready
The medical crew prepared for the transport by developing a plan based on the limited information received. Depending on the severity of the patient’s condition, the plan even included possibly taking the patient to the closest port of entry in the US, instead of their intended destination, if his condition was worse than what had been ascertained.
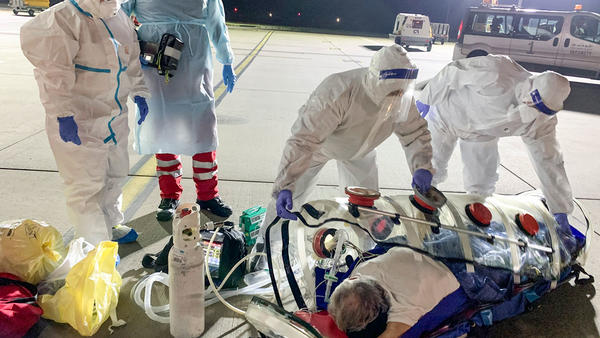
Once the aircraft landed in Mexico, the crew donned their hazmat suits to avoid any possible contamination. The patient was brought to the aircraft by the ground ambulance crew.
Inside the ambulance, the patient was found not sedated, not on a patient monitor, and actively being bagged by a bag valve mask without a PEEP valve. This, despite assurances the patient would be brought to our aircraft by a physician who would be managing a ventilator! Additionally, the ground ambulance crew was not taking Covid precautions.
Patient management
The patient was clearly anxious and in distress. The medical team quickly assessed the situation and immediately placed the patient on our ventilator and monitor. The patient presented with an oxygenation in the low 80s, a low systolic blood pressure and was very tachycardic. The team also ascertained that the patient was very dehydrated. They started an IV and gave a fluid bolus, which immediately increased the patient’s blood pressure. The patient continued to receive fluid hydration throughout the flight.
The patient had to be initially placed on 100 per cent FiO2 in order to bring his oxygen up to an acceptable level of greater than 90 per cent. After calculating oxygen consumption, the team determined they would not have enough oxygen to fly the flight non-stop to the final destination if the FiO2 remained at 100 per cent.
Since the patient was still over breathing the ventilator due to anxiousness, the crew decided to sedate and paralyze the patient to decrease his oxygen needs. Once the patient was paralyzed, the crew was able to decrease the FiO2 to maintain oxygenation in the mid to high 90s.
As the team medically managed the patient and performed critical and timely interventions, the patient continued to improve and was successfully transported non-stop to his destination. The quick actions by the AirCARE1 medical team ultimately averted a negative outcome for this patient and helped him on the path to an eventual full recovery.